Surgery for Cancer of the Vulva
The type of surgery carried out depends on the type, size, depth and position of the vulva cancer and your general health. The aim of the surgery is to remove all of the cancer and an area of healthy tissue around it (this is called a ‘margin’).
It is planned that you will have a Wide Local Excision (WLE) – a small area of the vulva is removed however the size and depth can vary.
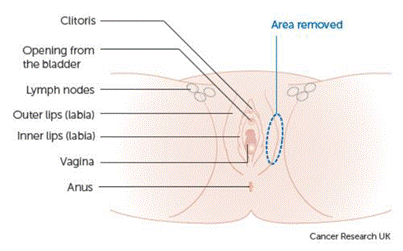
Is there any alternative to surgery?
You have the option not to have surgery for cancer of the vulva; your surgeon will discuss the alternative treatment options available to you.
What happens if I decide to have no treatment?
If you choose not to have treatment with surgery, radiotherapy and/or chemotherapy the health care professionals looking after you will discuss how best to support you with any ongoing difficulties. The nurses can refer you to a team in the community with specialist knowledge (District nurses/community Macmillan).
Risks and complications of surgery
There are risks and complications associated with any surgery, but the most common are listed below:
Anaesthetic
The surgery is usually carried out under general anaesthetic (this means that you will go to sleep). You will meet the Anaesthetist before your surgery who will explain the possible risks of the anaesthetic in more detail and the type of anaesthetic you will need.
Bleeding
You will have some bleeding at the time of your surgery and, although this is normally minimal, a blood transfusion is sometimes needed. Rarely, there may be internal bleeding after the surgery, making a second surgery necessary.
Infection
With any type of surgery there is a risk of developing an infection which may be in the chest, wound or urine. Chest infections are caused by bacteria or a virus. General anaesthetics affect the normal way that phlegm is moved out of the lungs. Pain or difficulty sitting upright after the surgery can mean that taking a deep breath or coughing is difficult. As a result of these two things, phlegm can build up in the lungs. Within the phlegm an infection can develop. It is importance to carry out regular breathing exercises to help you clear your lungs.
Wound infections are common after this type of surgery. The first signs of infection are pain around the surgical site, redness and/or a slight discharge. You will be reviewed daily by the ward team and prescribed antibiotics should they be required. You can assist by keeping the wound clean and dry, alongside the nursing staff and reporting any signs of infection as soon as you notice them.
Wound breakdown
Wound breakdown can be a common complication after wide local excision and may be due to the tightness in the surgical area where the tissue has been removed and the skin has been re-joined, it can also be related to infection. This can be managed routinely by the nursing staff on the ward and if required by district nurses in the community upon discharge. Should a wound open, we do not re-suture these wounds but allow them to heal by secondary intention (this involves leaving the wound open and allowing it to heal on its own over time). Once the nursing staff are happy that your wound can be managed at home you will be discharged, a District Nurse can be arranged if needed. In some cases, it can take some time for the wound to heal completely.
A patient with a chronic illness, an immune system problem, or sickness in the weeks prior to surgery may have a lengthier hospital stay and a more difficult recovery period as wounds in these patients often take longer to heal. Diabetics who have surgery typically have a longer healing time, especially if blood sugar levels are poorly controlled.
Deep Vein Thrombosis (DVT) or Pulmonary Embolism (PE)
Occasionally after surgery it is possible to develop a blood clot in the leg (DVT) or in the lungs (PE). Moving around can help prevent this. If you have difficulty with your mobility the physiotherapist can visit you after your surgery to give advice and to help with your mobility. We will give you special surgical stockings (known as ‘TEDS’) to wear whilst you are in hospital and we recommend that you wear them for two to six weeks depending on your surgery, your medical team will advise.
To reduce the risk of blood clots following your surgery you will be given injections (Tinzaparin) to thin your blood during your stay in hospital and for approximately 28 days after discharge. You will be shown how to give the injection to yourself, so you are able to give continue these at home once discharged. You will be given an information leaflet on discharge explaining how to prevent blood clots.
Patients who have had a DVT before are higher risk for getting another clot and should tell their doctor or nurse about this.
Possible consequences of vulva surgery:
Changes in bladder and bowel function
If your surgery requires removal of part of the urethra (tube that drains the bladder) or anus you may experience some difficulties passing urine or stool, these may be short term or long-term effects. Your surgeon will discuss this with you before your surgery.
Numbness/reduced sensation
Many patients experience numbness and tingling around their surgery site, for some it is a temporary condition; others find it may be longer term. Creating an incision requires the surgeon to cut through nerves, which send messages between the body and the brain. If enough nerves are cut, the area surrounding the surgical site may have numbness or a tingling sensation. Depending on the location of the damage, the nerve may regenerate, allowing sensation to return to the area over the course of weeks or months. In other cases, damage to the nerves may be too great for the body to repair, resulting in permanent numbness or tingling. Medication can be prescribed to help if numbness/tingling becomes problematic.
Changes to sexual relationships
After some surgery for cancer of the vulva, scar tissue may narrow the entrance to your vagina and can make it painful to have sexual intercourse. Some women who have had surgery to the vulva have a reduction in sexual desire or pleasure and may also have difficulty reaching orgasm. This is most likely if you’ve had your clitoris removed.
Top Tips
Following discussion with patients who have undergone this type of surgery they have suggested the following:
- Patients have reported certain types of clothing uncomfortable, recommending nightdresses rather than pyjamas (the ward can also supply nightdresses with open backs which can make movement, toileting and positioning easier and can also reduce the amount of laundry for your family).
- Patients have also purchased disposable net knickers which can be more comfortable and can cut down on laundry.
- Day clothes – patients have found long skirts more comfortable than trousers.
- Patients have found hospital toilet paper can be quite hard and suggest bringing your own soft toilet paper into hospital with you.
Hygiene/ Wound Care
It is important that you shower at least once daily to keep your wound clean. Your wound will be checked regularly for any signs of infection, and you will be advised how to care for your wound when you are in hospital. It is safe to get your wound wet unless otherwise advised. Avoid using scented products, lotions, perfumes, and talcum powders in the area of your surgery site until your wounds are fully healed. After washing, pat dry your wounds with a clean, soft towel (the ward staff can provide hospital towels to help cut down on your laundry). When resting on the bed we would advise wearing no underwear as exposure of the wound to the air will aid healing and will be more comfortable. When you become more mobile wearing loose-fitting clothing and wearing cotton underwear is advised.
It is very important that you clean and dry your vulva wound after toileting as increased moisture in the vulva area can lead to wound breakdown. Your vulva stitches are dissolvable and don’t need to be removed unless they become problematic. Vulva wounds can be very uncomfortable, and some patients find sitting for any length of time difficult. The ward can provide you with a special cushion to sit on, please ask if you feel you would benefit from using one.
Emotions
It is very common to feel tearful, upset, or low in mood after your surgery, this can be a reaction to your diagnosis, to the surgery and also sometimes due to being away from your family and friends. It is important to talk about your feelings and you might find it helpful to talk to the ward nurses or clinical nurse specialist to ease your worries.
Body image
Having vulva surgery can permanently change the outward appearance of the body, a change many patients find hard to come to terms with. You may want to look at the area but do not force yourself to do this before you are ready. However well prepared you are you may feel shocked, and this is perfectly understandable, because of the tissue that has been removed it may look very different. It may affect how you feel about your sexuality and womanhood, some patients find this surgery disfiguring and you may need a lot of support to help you through it.