What is Dupuytren’s Disease?
Dupuytren’s disease is a thickening of the deep tissues of the palm and fingers. The thickened tissue contracts over time, pulling the finger(s) towards the palm. Dupuytren’s contracture usually progresses slowly and may not be troublesome for years. This is a fairly common condition. Unfortunately, there is no way to stop or cure the problem completely, although many people will never need any treatment.
It may start with lumps, dimples or ridges, commonly at the base of the little and ring finger. In the initial stages the nodule may be uncomfortable, but Dupuytren’s is usually painless. Over time, the nodules may grow into cords of contracted tissue that pull the finger towards the palm and prevent it fully straightening. The disease may first be noticed when you are unable to put the hand flat on an even surface such as a table. Some people report difficulty with washing, wearing gloves or putting the hand into pockets.
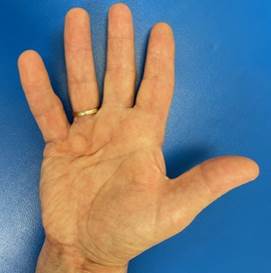
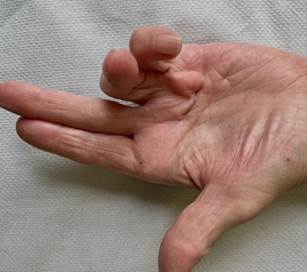
Who is affected?
The cause of Dupuytren’s contracture is not fully understood; it develops more often in men than women and is known to run in families. It usually arises in middle age or later life. It is associated with liver disease, diabetes, alcohol dependence and smoking, but many people who develop Dupuytren’s contractures have none of these factors. It may also occur following injury or surgery to the hand or wrist.
What are the treatment options?
The condition is progressive and results are generally poor if the fingers become very bent. There are several treatment options which include:
- Leaving it alone -this is best for mild deformities and in those with minimal functional limitation.
- Percutaneous needle fasciotomy -is occasionally indicated for patients with isolated deformity of the knuckle joint. It involves using a needle or knife to snap the band causing the deformity. Recurrence rates are high.
- Palmer fasciectomy -involves removing all visible Dupuytren’s tissue. A zig-zag incision is used to the palm and finger. If there is a severe contracture, a skin graft(taken from the medial forearm) may be needed. Fasciectomy surgery has the least recurrence rates.
- Dermofasciectomy -The surgeon will remove the whole cord as well as the skin over it. A skin graft is placed usually taken from the upper arm. Wound healing is longer.
- Amputation – used for severe contracture, nerve or blood vessel damage or for multiple recurrences.
What does the operation involve?
The aim of surgery is to reduce or correct the finger contracture, and therefore improve function. The procedure involves removal of the tight tissue band(s) causing the deformity. You will have one or more incisions in your hand, these wounds are usually stitched in a zig-zag manner.
Prior to surgery, please trim your nails and keep your hands clean, and remove any rings you might have on the operation side. Ensure you have someone to drive you home afterwards.
The surgery is done as a day case procedure under either a local anaesthetic which numbs the affected area or a regional anaesthetic which numbs the whole arm and you remain awake. On some occasions, it may be done as a general anaesthetic; for which you will be asleep. The type of anaesthetic will be discussed with you when you are listed for the operation.
What complications can occur?
Any surgical procedure has an element of risk. Specific complications of Dupuytren’s surgery include:
- Pain / stiffness – especially of the finger joints. The risk increases if you have arthritis in your fingers.
- Wound complications -wound complications may delay healing. Wound dehiscence can occur which is opening of the wound.
- Infection – at the surgical site. It is important to keep the dressings clean and dry after surgery.
- Incomplete correction -this is due to a joint contracture or extensive scarring forming post-operatively. Unfortunately, this can be difficult to treat.
- Neurovascular nerve injury – There is an increased risk of damage to the nerves and blood vessels during operations, as nerves of the hand can be entwined around the cord. This may result inpermanent or temporary loss of sensation (feeling), including numbness in the finger(s). It is quite common to have temporary loss of feeling in the finger(s) for up to 6 weeks or more.
- Recurrence -since the disease cannot be cured, recurrence may occur at the site of surgery or elsewhere in the hand. The rates of recurrence are on average 50% over 10 years but majority do not need further surgery.
- Cold intolerance
General complications associated with surgery include:
- Bleeding/swelling – to minimise this, it is important to keep the hand elevated during the first 48-72 hours following surgery.
- Delayed wound healing -often the skin takes more than two weeks to heal fully. If this is the case, you may need frequent wound checks until it is healed. If skin grafts are used, they may not fully take.
- Scar tenderness -this normally subsides by 6 weeks but may persist for up to 3 months. Massage to the scar can be helpful to relieve these symptoms once the scar has fully healed.
- Chronic regional pain syndrome (CRPS) -a rare complication. This can cause pain, stiffness and swelling of the hand which may be permanent. It is often difficult to treat (less than 10%).
- Amputation of the finger – rare complication.
What happens before the operation?
Pre-admission assessment
If you have a regional or general anaesthetic, you will attend a pre-assessment clinic. This is an assessment of your health to make sure you are prepared, for your admission, treatment and discharge. Please bring a list of all your current medication including a list of allergies and the type of reactions. Before the date of your admission, read very closely, the instructions given to you by the pre-admission assessment and your appointment confirmation letter.
Planning ahead
Once you have your date for surgery, you can do several things to aid preparation for your operation and to improve your recovery.
It is important to plan and arrange for how you will manage when home. Stocking up your freezer with easy cook items is advised (particularly if you live alone), as you may find daily tasks such as cooking more difficult initially after your operation. If you have family or friends, who can stay with you or visit regularly, this may make your recovery easier both for helping with household tasks and moral support.
Smoking
Smoking has been shown to delay wound healing and increase complications after surgery. Patients, who stop smoking benefit from long-term improvements to general health, decrease the risks associated with anaesthetic and may have a better outcome from the operation. If you are interested in stopping smoking, please speak to your pre assessment nurse or GP for advice and services available.
Weight
Even though you may feel fit and healthy at your current weight, patients with a higher body mass index are most likely to experience potential serious complications both during and after surgery. If you are keen to lose weight, please speak to your GP or pre assessment nurse for services available.
Cancellation
If you are unable to attend your appointment, please contact us immediately so that we can offer your appointment to another patient.
Your surgery
Day of surgery
You will be given specific instructions about when to stop eating and drinking, please follow these carefully, otherwise this may pose an anaesthetic risk and we may have to cancel your surgery. You should have a bath or shower before coming in to hospital. The anaesthetist, surgeon or a member of the team will visit you prior to the operation, and can answer any questions. You will be asked to sign a consent form.
Post operation care
After your operation, your hand will be in a bulky dressing, this maybe a ‘boxing glove dressing’. You will be given an arm sling to reduce the risk of bleeding or swelling. You will be seen the following week for a wound review and a dressing change with sutures being removed at 12-14 days after surgery. This maybe at your GP practice or within a hospital orthopaedic/dressings clinic. You will be notified of this.
It can take between 4 – 12 weeks to recover after palmar fasciectomy surgery. Your wounds should heal within a few weeks but full recovery may take many months.
Things to do after the operation
- Ensure to elevate your hand (higher than the elbow) after the operation to control the swelling, this is especially through the night. You can support your hand on cushions when you are sitting in an elevated position
- Avoid walking with your hand down by your side as this may cause pain and increased swelling
- Always keep your dressing dry (wear a bag over your hand when showering)
- You are encouraged to move your hand and wiggle your fingers after your operation, even with your stitches in, this can help to prevent complications of joint stiffness (see exercises)
- You may experience stiffness and scar tenderness with discomfort/pain following surgery, this can usually be controlled by simple painkillers
- Normal light use of the hand is encouraged especially once the wound is fully healed. Heavy and repetitive use should gradually be introduced once the wound has healed and you are able to move your hand normally
Contact us or your GP if
- If you have severe pain, excessive swelling or bandages that are too tight or have excessive blood
- If your fingers become cold, blue or numb
- You suspect a wound infection or have wound complications
Physiotherapy
Not everyone is referred to physiotherapy after the operation; the surgeon will recommend this if they feel you need it. If you are struggling with moving or using your hand after surgery, then please get in touch with us on the telephone numbers at the end of this leaflet.
You will not routinely be given night splints unless the surgeon recommends. Studies suggest these do not improve the correction achieved for the majority of patients. If you are provided with a night splint, these are normally worn between 4-6 months after the surgery.
Scar Massage
Once the stitches have been removed and the wound has fully healed, you can start scar massage. It can be common for the scar to become lumpy, firm, tender and pink, which can be helped by massaging the scar and surrounding area firmly. You can use non-perfumed moisturising cream such as E45, aqueous or Vaseline.
Exercises
Your hand will be in a dressing that is applied in theatre, this can be bulky. Bend and straighten your fingers and wrist within the constraints of this. Also, ensure you are bending your elbow and moving your shoulder.
The dressing will be changed and a lighter dressing applied within 1 week after having the operation. Continue to bend and straighten your fingers more within the constraints of this dressing.
The sutures will be removed 12-14 days after the day of your operation. You should now be able to move your fingers more, the aim is to bend your fingers to your palm and make a fist. Straighten your fingers as able.
Tendon gliding exercises
Start these exercises as soon as you can, once both the dressing and stitches have been removed. You may find this exercise difficult initially, but it will become easier once you can move your finger(s) more. Repeat sequence 4-6 x per day, 5-10 repetitions eachday, 5 to 10 repetitions each
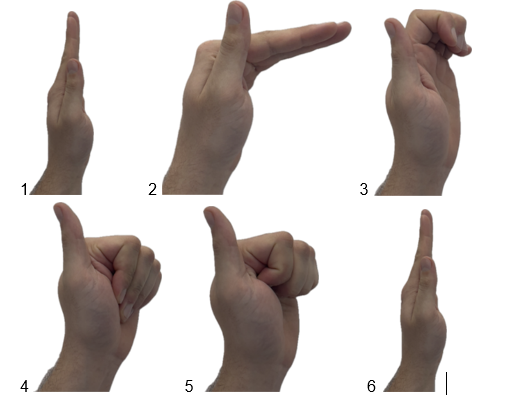
1. Fingers straight
2. Bend the knuckles
3. Hook fist – knuckles straight, fingers bent
4. Flat fist – tips of fingers straight
5. Aim to make a tight fist
6. Fingers straight
Finger & Thumb Exercises
Continue to try to make a full fist with your affected hand.
If you are unable to do this, push the fingers of your affected hand into a fist using your unaffected hand. Ensure all 3 joints of the fingers are bending. Hold position for 5-10 seconds. Repeat 5-10 times.

Once the stitches have been removed and the wound is healing. With your other hand gently try to straighten the operated finger(s). Care must be taken not to force this. Do not overstretch into pain.
Hold position for 5-10 seconds. Repeat 5-10 times.

Oppose your thumb to each of your fingers. Repeat 5-10 times.

Physiotherapy locations
Should you be referred to physiotherapy, depending on the location of your GP, the physiotherapy provider may be different.
- If you have a Gateshead / Newcastle GP, your physiotherapy provider will be Tyneside Integrated Musculoskeletal Service (TIMS). If you have a query about your first appointment with TIMS, please contact the booking team on 0191 445 2643
- If you have a Durham GP, your physiotherapy care will come under Durham. Please contact the Queen Elizabeth hospital, physiotherapy department should you not receive your first appointment on 0191 445 2320
- If you have a GP that is outside of the Gateshead / Newcastle or Durham area and you have had elective surgery, your physiotherapy will be at the Queen Elizabeth hospital. Should you not receive your first appointment, please contact physiotherapy reception on 0191 445 2320
When can I resume normal activities?
Driving
Once your wound has fully healed and you can make a full pain free fist. Usually 3-4 weeks. Notify your insurance company.
Washing up / Swimming
Avoid until the wound is fully healed. You may need to use a rubber glove initially with washing up as your hand may be a little sensitive to the heat of the water. Usually 3-4 weeks.
Work
Your return to work will be dependent on your recovery following surgery and the nature of your job. Most people return to office based work by 2-3 weeks and for more physical work up to 6-8 weeks. Obviously this may vary depending on your job, hand dominance, any complications and the rate of recovery of hand function.
Where can I go for more information?
NHS: Dupuytren’s contracture – NHS (www.nhs.uk)
NHS England: NHS_Dupuytren’s_contracture_decision_tool (england.nhs.uk)
FAQs: https://dupuytrens.org/faq/
Patient Info: https://patient.info/bones-joints-muscles/dupuytrens-contracture-leaflet
British Dupuytren’s Society: https://dupuytrens-society.org.uk
Telephone numbers
| During the hours of 8am to 8pm contact the Day Surgery Unit, Peter Smith Surgery Centre, Queen Elizabeth Hospital | 0191 445 3009 |
| During the hours of 8pm to 8am contact Level 3, Peter Smith Surgery Centre, Queen Elizabeth Hospital | 0191 445 2028 |
| During the hours of 8am to 4:30pm contact the Physiotherapy Department | 0191 445 2320 |
| During the hours of 8am to 8pm. If you have a Gateshead or Newcastle GP, TIMS will be your physiotherapy provider If you have a query about your first appointment with TIMS please contact our booking team on 0191 445 2643 If you are a current TIMS patient and have a query about your follow-up appointment please contact our local admin team on 0191 213 8800 | Booking Team: 0191 445 2643 Local Admin Team: 0191 213 8800 https://www.tims.nhs.uk/ |
| Main Switchboard | 0191 482 0000 |