This booklet is for patients who have had hip replacement surgery at Gateshead Health NHS Foundation Trust.
Inpatient length of stay
We aim to get you home as soon as possible following surgery once all discharge goals have been achieved and you are medically well. This is usually 1-2 nights after surgery.
Some patients may be suitable to have day case surgery which will be discussed prior to admission. This means you may be discharged on the same day as surgery.
Hip Precautions
Hip precautions are used to keep your hip joint in safe positions that will help prevent dislocation while the soft tissue around the hip is healing.
The following precautions are to be followed for 6 weeks after surgery:
- Do NOT bend your hip past 90°
- Do NOT move your leg across midline (e.g. no crossing legs, lie on your back in bed)
- Do NOT twist when standing
Goals of initial rehabilitation:
- Restore hip range of movement (within hip precaution ranges)
- Regain strength
- Reduce swelling
- Adequate pain control
Discomfort
Post-operative pain, swelling, and bruising are a normal part of the recovery process following joint replacement surgery. The muscles and tissues surrounding your hip will take time to heal. You will require pain relief medication on a reducing basis, usually over at least 6 weeks following the surgery. Crutch use, ice, activity pacing and rest may help.
Increased discomfort at night and difficulty sleeping is very common following a hip replacement, this should improve with time.
Following your discharge from hospital; you need to apply the ice pack three to four times daily for 15-20 minutes. You will be able to reduce the frequency after this time but will find that you will benefit from ice therapy for up to three months to help manage the pain.
If you have any concerns regarding managing your pain, please discuss this with your GP.
Swelling
Swelling and inflammation is a normal part of the healing process. This can last up to a few months or longer but will improve with time. Swelling of the leg is different for everyone and may cause the leg to ache and feel very heavy.
Swelling, either around the knee/hip, or throughout the whole leg, is normal. It can worsen once you return home, as you start to do more.
Bruising may appear near the operation site and may then travel throughout the leg (from hip to knee). This is quite normal and may remain for a couple of weeks.
Elevating your leg on a stool or on the bed will also help manage the swelling.
When should I seek help?
You should see your doctor urgently if you:
- Have a sudden increase in severe pain, swelling or tenderness in the calf which is getting worse and not just related to pain expected while performing the exercises.
- Have concerning pain, swelling or tenderness in the joint which is getting worse.
- Develop a high temperature and feel unwell.
- See fluid, pus or blood coming from the wound.
- Develop new numbness or tingling near to the joint.
Mobility and Walking Aids
After your operation, it may be necessary for you to use crutches to help you walk. Your physiotherapist will provide you with a pair of crutches and show you how to use them.
Everyone is different as to when they stop using crutches; this often depends on your previous level of mobility. When you feel confident with your elbow crutches and you are able to walk without a limp, it is recommended you progress to using only one crutch in the hand on the opposite side of your surgery.
For example: if you have a left hip replacement, use your elbow crutch/stick in your right hand.
Once you are no longer using your crutches; please return them to the hospital. You will be provided with further guidance from the outpatient physiotherapy staff as to when it is appropriate to gradually stop using elbow crutches.
Stairs / Steps
Going up stairs with a rail
Keep your crutch/es on the step you are standing on.
Step up with your un-operated leg, then your operated leg and then bring your crutch/es up onto the same step.

Going down stairs with a rail
Put your crutch/es down first into the middle of the step below. Step down with your operated leg and then follow by your un-operated leg.

Going up stairs without a rail
Keep your crutches on the step you are standing on.
Step up with your un-operated leg, then your operated leg and then bring your crutches up onto the same step.

Going down stairs without a rail
Put your crutches down first into the middle of the step below. Step down with your operated leg and then follow by your un-operated leg.

Exercises
It is important that you continue doing the exercises that have been given to you by the physiotherapist on the ward. These exercises should be completed three to four times a day.
It is normal to experience additional discomfort whilst doing these exercises and for up to an hour afterwards.
Prior to commencing exercise, it is advisable to take adequate pain relief to optimise the benefit of these exercises. Especially if you are finding them difficult. Then use ice following completing your exercises.
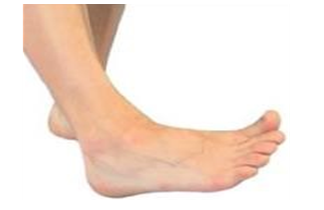
Ankle Rotation
Lyingor sitting: rotate your ankle in circular movement
Repeat 10-15 times, 3-4 times a day
Hip abduction (lying)
Lying on your back; slide your leg out to the side. Keep your body straight throughout the exercise
Repeat 10 times, 3-4 times a day

Hip Flexion
Lying on your back; bend knee slowly towards you then straighten maintaining good control
Repeat 10 times, 3-4 times a day

Bridging
Lying on your back; with both knees bent and feet on the bed.
Lift your pelvis and lower back off the bed.
Hold for 5-10 seconds, Repeat 10 times, 3-4 times a day

Seated Quads
Sit in a chair, pull your toes up towards you and tighten your thigh muscles to straighten your knee slowly.
Hold for 5-10 seconds, Repeat 10 times, 3-4 times a day

Abduction
Holding onto a chair or kitchen bench:
lift your operated leg to the side keeping your foot pointing forwards.
Hold for 5-10 seconds, Repeat 10 times, 3-4 times a day

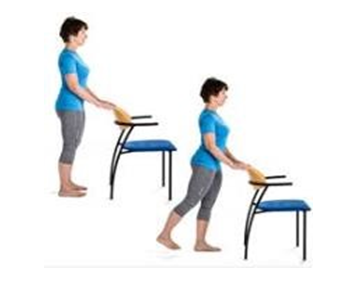
Extension
Holding onto a chair or kitchen bench:
stretch your leg out behind you keeping your body straight.
Hold for 5-10 seconds, Repeat 10 times, 3-4 times a day
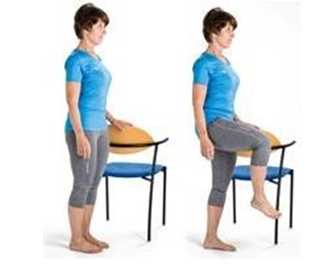
Flexion
Holding onto a chair or kitchen bench:
Stand upright and slowly bend your knee and hip in front of you.
Hold for 5-10 seconds, Repeat 10 times, 3-4 times a day
Please follow this link to watch ‘ Joint Care Clinic – Hip Exercises’
Follow up
You will have an appointment in the orthopaedic clinic 6-8 weeks after your procedure.
Transport
If you require an ambulance for transport to the group; you will be provided with a telephone number to ring and arrange this. This will be sent out with your physiotherapy appointment letter.
Community Rehabilitation
Occasionally people are discharged home using a walking frame. If appropriate; the ward physiotherapist may need to make a referral to the community team to review and progress rehabilitation at home. You will be contacted by either telephone or letter to advise when a visit can be arranged.
Please note: If you have not received notification of your follow up physiotherapy appointment/s within 2 weeks of leaving hospital, please ring 0191 445 2320 so we can check your referral.
Work
Returning to work will be dependent on the demands of your job. This will be guided by your surgical team and physiotherapist. This will be sooner if you have a sedentary / desk based job. If you have a heavy manual job you may require longer off work. You can discuss this with your GP or Consultant if you are not sure.
Driving
You will not be able to drive for at least 6 weeks following your operation. Once you are able to walk without any mobility aids you can drive when you feel safe to do an emergency stop and safely control a car. You must tell your insurance company that you have had knee surgery. If in doubt, contact your consultant or GP.
Telephone Numbers
If you are at all worried by your knee please contact us:
| During the hours of 8am – 8pm contact the Orthopaedic secretaries | 0191 445 8500 |
| During the hours of 8pm – 8am contact the Peter Smith Surgery centre, Queen Elizabeth Hospital | 0191 445 2028 |
| During the hours of 0800 – 16:30 contact the Physiotherapy Department | 0191 445 2320 |
| During the hours of 8am-8pm. If you have a Gateshead or Newcastle GP, the TIMS will be your physiotherapy provider. If you have a query about your first appointment with TIMS please contact our booking team on 0191 445 2643 If you are a current TIMS patient and have a query about your follow-up appointment please contact our local admin team on 0191 213 8800 | Booking Team: 0191 445 2643 Local Admin Team: 0191 213 8800 https://www.tims.nhs.uk/ |
| During the hours of 8.30am-12pm and 1-4pm. If you have a Durham GP, the County Durham Integrated MSK Service will be your physiotherapy provider. | Central booking team: 01388 455 200 |
| Main Switchboard | 0191 482 0000 |