Why do some couples need egg donation?
There are a variety of reasons why some women may not be able to produce their own eggs or produce enough good quality eggs during IVF (in vitro fertilisation).
The most common reasons are: –
- Women born without ovaries or with under-developed ovaries
- Women whose ovaries stopped working prematurely
- Women whose ovaries have stopped working due to radiotherapy, chemotherapy or after surgery
- Women undergoing infertility treatment but whose ovaries consistently produce poor quality eggs when stimulated
- Women undergoing infertility treatment but whose ovaries do not respond to fertility drugs
- Some women may not wish to use their own eggs as they may be carriers of genetic a disease such as haemophilia
Under these circumstances the best option is egg donation.
Who can become an egg donor?
Women who are considering becoming egg donors should be in a stable relationship, have already had children and have preferably completed their own family. Egg donors should ideally be less than 36 years old. Donors may be a friend or relative of the woman who needs egg donation.
All egg donors will go through a series of screening procedures, this will include a detailed medical and family history. Blood tests will also be performed including AMH level (which is a measure of how the ovaries may respond) and to screen for infectious diseases. These include Hepatitis, HIV, Syphilis, Gonorrhoea and Chlamydia screening. A blood test will also be carried out to check if the donor is immune to a virus called cytomegalovirus (CMV). This virus produces a mild flu like illness in adults but if caught when pregnant it can cause abnormalities in the developing baby. If the donor is immune to CMV they should be matched with a recipient who is also immune to CMV.
Donor’s blood is also tested for the risk of cystic fibrosis and genetic problems (karyotype).
Patients from different population groups, may need to be screened for other genetic conditions such as Tay-Sach’s diseases, Sickle Cell Anaemia and Thalassaemia.
It is important to remember that any tests carried out may reveal previously unsuspected conditions that may have implications for you and your family.
Donor Anonymity
The law changed in April 2005 to require that egg and sperm donors must be identifiable. This means that any children born as a result of donation will be able to access the information about the identity of their donor at the age of 18. This new regulation will not apply retrospectively to anonymous donors from before April 2005.
The law was changed as it was felt that children born from donations should have access to information about their genetic origins.
Identifiable donors should be reassured that attempts will be made to contact them before their identity is disclosed to a donor conceived person. It is important that up to date details are maintained to facilitate this. All details are held on the HFEA Register.
How does egg donation work?
As an egg donor you will undergo a cycle of treatment that is of IVF.
In an egg donation cycle the donor is given a course of drugs to stimulate the ovaries into producing eggs. The eggs are then taken out of the body and fertilised in the laboratory with the sperm from the husband, partner, or donor of the recipient. Normally a single fertilised egg (which are called embryos) are then replaced in the uterus (womb) of the recipient.
What are the procedures, drugs and side effects?
Downregulation
Downregulation involves switching off the pituitary gland. The pituitary gland produces hormones to control the menstrual cycle. We need to switch off these hormones to stop them interfering with the IVF cycle. Downregulation must be continued until day of trigger injection (36-38 hours before egg collection).
Risks and Side Effects
Because the downregulation drugs switch off your hormones, you may experience a number of menopausal-like symptoms, such as hot flushes, irritability, and headaches.
Immediately after starting the downregulation drugs, a burst of your own hormones may be released this could increase your fertility for a few days with the risk of a multiple pregnancy. It is therefore advisable that you use contraception until your next period or scan.
Medication
The types of drugs used in downregulation are:
- Nafarelin (Synarel)
- This is a nasal spray. The usual dose is to take two sniffs in the morning and two sniffs in the evening.
- Buserelin (Suprefact)
- This is a daily injection, which we can teach you how to give yourself.
The down regulation drugs can be started on day 21 of your cycle if you have regular periods or day one of your cycle if your periods are irregular or on a specific date given to you from the unit. You will need to be taking the drugs for at least two weeks when we will perform a scan. All scans for infertility treatments are performed via an internal scan which is placed a short way into the vagina. This type of scan gives us very good pictures of the uterus and the ovaries.
If your hormones have been switched off, the lining of the womb (endometrium) should be thin, and the ovaries should appear inactive. If this is not the case, then you may have to stay on the down-regulating drugs for a further 1 – 2 weeks when a rescan is performed. If your scan shows that your hormones have been adequately switched off then you are ready to proceed to the next stage of the cycle which is called superovulation.
Step By Step (Down Regulation)
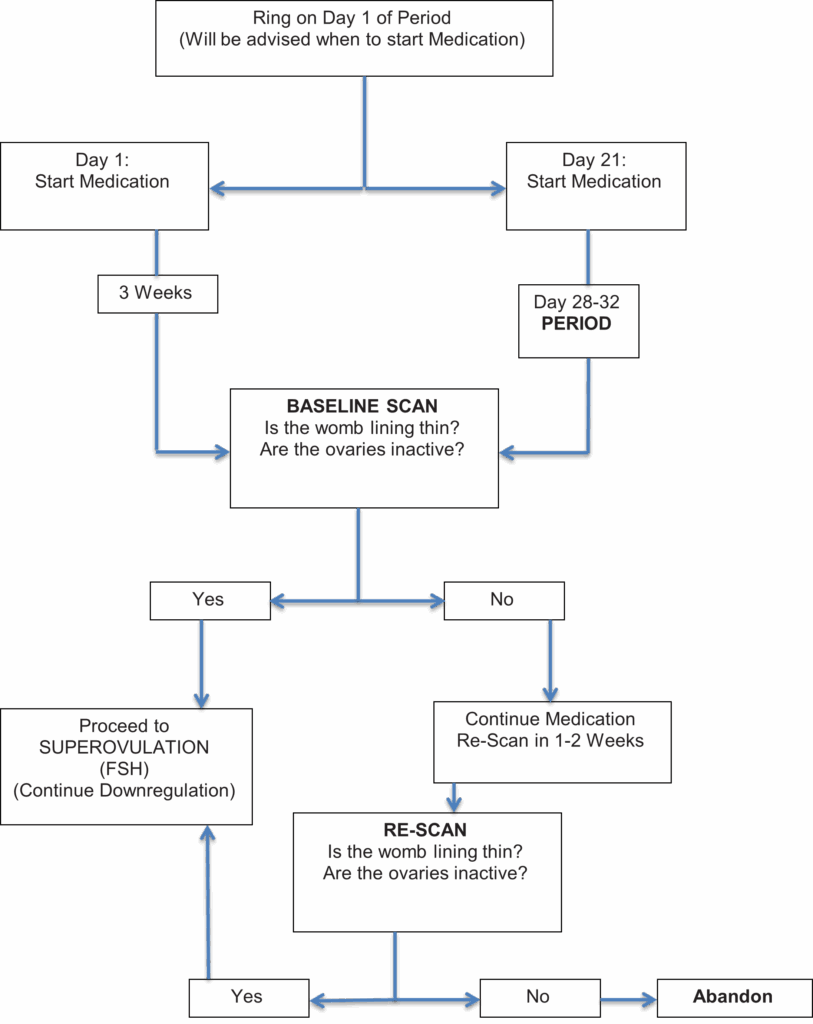
NB. If the lining of the womb is thickened and the ovaries are active, the cycle will be delayed, downregulation will continue, and a scan rescheduled.
Superovulation
During this part of the cycle, we use fertility drugs to stimulate your ovaries into producing a number of eggs.
It is important you continue the downregulation drugs during this part of the cycle.
The type of drug used in superovulation is a hormone called follicle-stimulating hormone (FSH) and we may use Ovaleap or Meriofert. This is a daily injection. The choice of drugs will be discussed with you before your treatment and is determined by your AMH result.
It is essential that we monitor the growth of these egg follicles, and we do this with the day six and day ten scans.
Follicles are a small cyst like structure on the ovary which contains the egg.
Risks And Side Effects
You will be taught how to give yourself your injections. You may experience some bruising at the injection site. The aim of superovulation is to stimulate the ovaries into producing follicles. If too many follicles develop you may develop Ovarian Hyperstimulation Syndrome (OHSS). This is discussed in detail later in this booklet.
Step By Step (FSH)
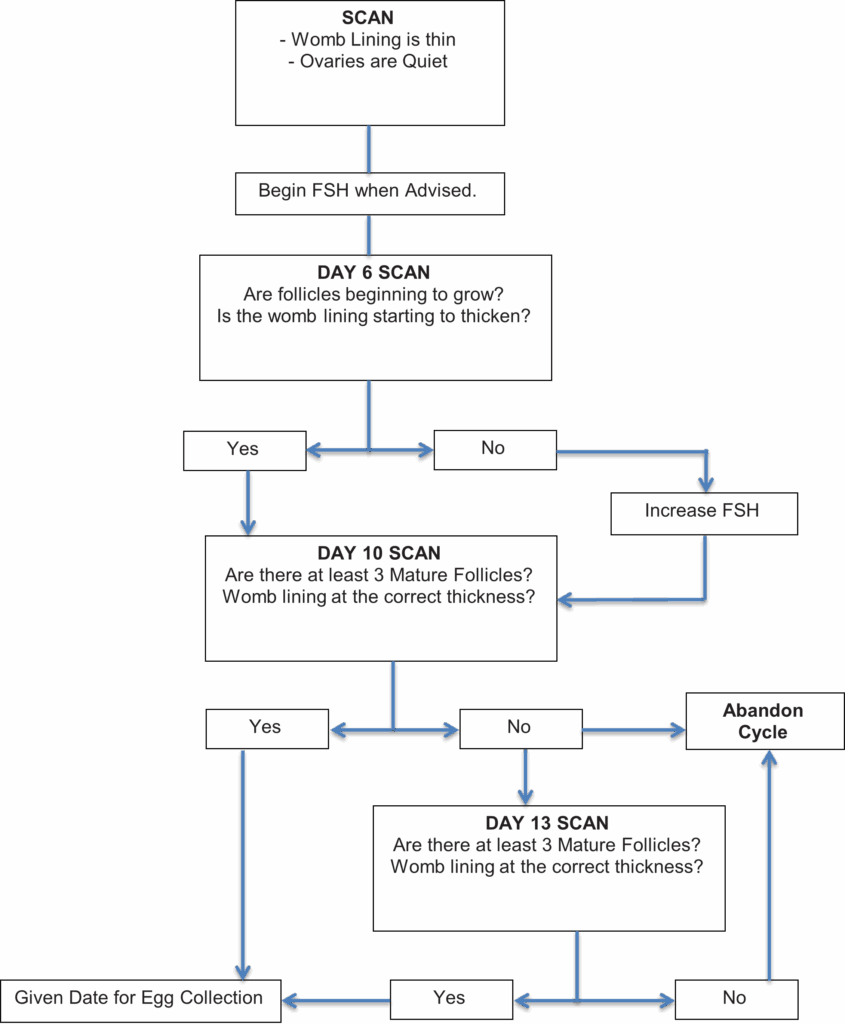
Egg Collection
The procedure itself is performed using the vaginal scanner with a fine needle attached. The needle is passed into each ovary and the fluid filled follicles containing the eggs are drained. On average an egg is collected from 80% of follicles. The whole procedure lasts 15 minutes and there is a possibility of experiencing some discomfort or pain during the procedure to counteract this you will be given a mixture of sedatives and painkillers. Once collected, the eggs are washed and stored in the incubator.
You will be able to leave approximately two to three hours after the egg collection you will need to be driven home as the drugs can cause drowsiness.
The embryologist will then prepare the sperm and add it to the eggs that have been collected. Usually five days later (can occasionally be three) if fertilisation and division have taken place the embryos are then replaced in the recipient’s womb.
Problems That May Occur
We may not be able to collect eggs due to a failure to respond to the fertility drugs or a technical difficulty in collecting the eggs (very rare).
Ovarian Hyperstimulation Syndrome (OHSS)
Some degree of ovarian hyper-stimulation occurs in all women taking fertility drugs. However, when this over-stimulation is excessive it can lead to problems. This occurs in about 7% of women and in 2% it may be sufficiently severe to need hospital admission.
OHSS develops when the ovaries produce too many eggs and swell up extensively. Blood vessels that supply the ovaries can leak fluid into the abdomen and cause the tummy to swell, leading to abdominal pain. Other features of the condition include vomiting which leads to dehydration. The dehydration may be made worse by fluid leaking out of the circulation, causing the blood to become concentrated. This can lead to blood clots and kidney problems. If this fluid collects in the chest it may cause shortness of breath.
OHSS may occur while taking the Ovaleap or Meriofert injections (if this occurs before the HCG injection we may stop your treatment to protect you from the effects of severe OHSS.
(YOU MUST NOT HAVE SEXUAL INTERCOURSE UNTIL YOUR NEXT PERIOD)
OHSS may also occur after the HCG injection – we will still collect the eggs.
It should be stressed that severe OHSS is very rare. And even in severe cases the condition is usually self-limiting and settles after a few days.
Contact Us
If you’re worried you are developing OHSS during your treatment you MUST contact the unit immediately
Telephone: 0191 445 2768 (Direct Line)
Email: [email protected]
or in the case of an EMERGENCY please call 0191 482 0000 and ask for a member of the IVF on call team after office hours.
Operative Complications And Infection
IVF does involve invasive surgical procedure and is therefore not without risk. The major risks relate to bleeding at the time of the egg collection and possible pelvic infection afterwards. The incidence of both of these complications is thankfully very low.
As it is unlikely that we will collect all the eggs it is very important that you take contraceptive precautions during the egg donation cycle.
What is the legal situation?
As the person donating the eggs you will not be the legal parent of any resulting offspring. The Human Fertilisation and Embryology Act passed by Parliament (1990) define the mother as the woman who carries or gives birth to a child and her husband or partner as the father or legal parent. At the time of the donation, you relinquish all legal rights and claims over any offspring that may result from the donated eggs and all duties towards the child or children.
If a child born from your donation is disabled in any way you will not be held responsible, however, it is your responsibility to inform us of any genetic or inheritable diseases which present themselves in your immediate family (section 35, 1990 HFEA). The Congenital Disabilities (CivilLiability) Act 1976 enables a child to bring a civil claim for damages against another person whose wrongful act caused that disability. The legislation does not impose criminal liability.
Will I be given counselling?
The guidelines issued by the HFEA states ‘that skilled and independent counselling by someone other than the medical practitioner involved in the procedure must be available to the donor’.
The independent counsellor attached to the unit will conduct the sessions.
We require that, as a known donor, implications’ counselling is provided for a minimum of 4 sessions, these sessions are compulsory:
- Recipient couple together
- Donor alone
- Donor with partner (if applicable)
- All parties concerned
At this unit we offer free independent counselling. You should ensure that you are given and have understood sufficient information to make an informed decision. These sessions are performed via video link at a time arranged between yourself and the counsellor.
Egg Donor Payment
As an egg donor you can receive compensation of up to £750 per cycle of donation, to reasonably cover any financial losses incurred in connection with the donation, with the provision to claim an excess to cover higher expenses (such as for travel, accommodation, or childcare).
If you are an egg donor who is not a permanent resident of the UK you may be compensated in the same way as a UK donor, but you will not be able to claim an excess to cover overseas travel expenses.
If you are in doubt about any part of the procedure, before, during or after your donation and the ethical aspects involved, please feel free to ask questions or call the unit 0191 445 2768.