This leaflet explains about carpal tunnel, what it is and how it can be treated. It is intended for patients who are either thinking about or have decided to have surgery and aims to help you understand and gain the maximum benefit from your operation.
What is the carpal tunnel?
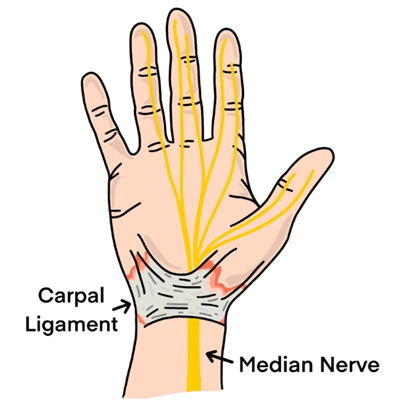
Carpal tunnel syndrome (CTS) is a painful condition that is caused by pressure on the median nerve, which travels from your forearm across your wrist, through the carpal tunnel. The carpal tunnel is a narrow passage surrounded by 8 small carpal bones and ligaments which lie below a tough band of fibrous tissue being the transverse (palmar) carpal ligament. It is the most common entrapment neuropathy.
The median nerve is responsible for sensation to the thumb, index, middle and a portion of the ring finger. It also supplies the short muscles of the thumb (thenar muscles).
Symptoms of CTS
The symptoms of carpal tunnel can vary from mild to severe. This can cause symptoms of pain, tingling (paraesthesia) or numbness. It may also cause weakness of the thumb which leads to dropping objects. Many people have gradually increasing symptoms which occur over time with muscle wasting at the base of the thumb in more longstanding cases.
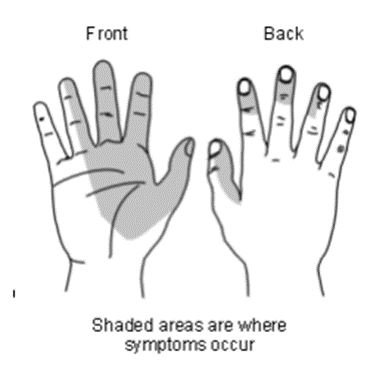
- Mild symptoms -intermittent tingling in the fingers, pain, worse at night, occasional clumsiness
- Moderate symptoms – symptoms are the same as for mild but are getting worse and affecting your work or activities. Tingling can be present most of the time with occasional numbness. Weakness in the thumb and dropping things but no flattening (wasting) of the thumb muscles on the palm side
- Severe symptoms – increased pain, numbness in the fingertips with difficult doing fine work. Flattening of the thumb muscle with weakness
What causes CTS?
The median nerve may become compressed within the carpal tunnel due to increased pressure. In most cases the cause of carpal tunnel is unknown. It is more common in women between the ages of 40-60 years but can occur at any age. Other risks include:
- Metabolic conditions i.e., diabetes, underactive thyroid
- Wrist fractures
- Obesity
- Pregnancy
- Genetic variations in the anatomy may predispose you to CTS
- Occupational exposure – use of vibration tools, repetitive movements of the wrist
- Inflammatory conditions like rheumatoid arthritis
- Changes within the hormonal level of the body, ie menopause
- Smoking
What are the treatment options?
The treatment options for carpal tunnel include:
- Do nothing – mild carpal tunnel symptoms often get better without any treatment. This is especially if you haven’t had symptoms very long and if you are pregnant. You need to monitor your symptoms and seek additional help should these become worse.
- Conservative management – you could stop or reduce activities for a short period that could be causing CTS like, repetitive bending your wrist, gripping something hard and using vibration tools. You can trial a wrist splint both during the day during activities for short periods and using a splint at night for bed. The purpose of a splint is to stop bending the wrist and they can be trialled for 4-8 weeks. You can also try painkillers, which may help to manage the symptoms in the short term.
- Steroid Injections – this is where a small amount of steroid is injected into the carpal tunnel aiming to reduce any inflammation. There is a variable success rate with steroid injections and we cannot predict who will have a successful response and your symptoms may still return. The option of a steroid injection will be discussed with you.
- Carpal tunnel release surgery – this may be offered to you if the above options have failed, you have severe symptoms or nerve conduction tests show you have nerve damage or muscle wastage.
Surgical procedure
Carpal tunnel decompression surgery is done under local anaesthetic and as a day case procedure, this means you can go home on the same day. The surgery is done in theatre either by a consultant or a member of the surgical team. This includes registrars and surgical care practitioners.
The procedure usually takes between 20-30 minutes and you will be awake. You will have an injection of local anaesthetic around your wrist to numb the area. You may feel some pressure during this procedure but you should not feel pain. An incision of 2-3 inches is made at the base of your palm and the tissues below the skin are cut and moved aside, until the transverse carpal ligament is identified. Using a scalpel, the transverse carpal ligament is cut, to release the pressure on the nerve.
The incision site is closed using internal stitches and your hand will be placed in a dressing with a wool and crepe bandage or a large boxing glove type dressing. You will be advised when to remove this which is typically between 48-72 hours. It is important to keep the wound dry until your wound check. The local anaesthetic will usually last for a few hours but some people may still feel the effects the next day.
Surgery usually improves symptoms of night pain and tingling within a few days although full recovery may take up to 1 year. This can depend upon the severity of symptoms. The wound should heal within 3-4 weeks. It generally can take up to 3 months to regain full strength and a fully comfortable scar. You will not be able to drive after surgery, ensure you have someone to accompany you home after the operation.
Are there any complications with this operation?
All surgical procedures are associated with a degree of risk. The main complications for carpal tunnel are:
- Pain It can be common to experience pain over the surgical site and in the muscle areas either side of the scar (pillar pain), this can be tender to touch or when you place pressure through the palm. The symptoms tend to be temporary but usually settle within 3 months. On occasion, it may take up to 6 months to improve.
- Scar sensitivity – is a common complication after CTS. It is normal for the scar to be sensitive at first but this normally settles down within 4-6 weeks, although in some instances, sensitivity may take up to 3 months for it to improve. The scar usually fades over time but will never disappear.
- Stiffness may occur in your fingers following any surgery. You will be encouraged to get your fingers moving as quickly as possible after the operation to minimise this risk.
- Incomplete relief of symptoms -some people do not always get full relief of their symptoms after the operation (1 in 20). This can be partly due to the severity of the nerve compression. In severe cases, improvement of constant numbness and muscle weakness may be slow or incomplete.
- Infection – the risk of infection is low in CTS (less than 7 in 1000).
- Neurovascular nerve injury – this is a rare complication (2 in every 1000). Since the surgery involves working close to the nerve, should there be an accidental injury to the nerve or one of its branches, it may lead to numbness, pain or weakness within the hand. These nerves can be repaired, although the extent of recovery is unpredictable.
- CRPS (Complex regional pain syndrome) – this is a debilitating condition that causes high levels of pain (which tends to be out of proportion to what you have had done), stiffness and swelling in the hand after surgery. It can be treated with special pain relief and physiotherapy, although it can take a long time to recover from it. It is a rare complication and can be identified in 2-5% of patients after carpal tunnel surgery.
- Reoccurrence – carpal tunnel symptoms can recur over time. For some people revision surgery may be required (30 in every 1000).
- Bleeding is usually not significant. If you take blood thinners please mention this to your surgeon or a member of the team prior to the operation.
What happens before the operation?
Planning ahead
Once you have your date for surgery you can do several things to aid preparation for your operation and to improve your recovery. It is important to plan and make arrangements for how you will manage when home. Stocking up your freezer with easy cook items is advised (particularly if you live alone), as you may find daily tasks such as cooking more difficult initially after your operation. If you have family or friends who can stay with you or visit regularly this may make your recovery easier both for helping with household tasks and moral support.
Smoking
Smoking is shown to delay wound healing and increase complications after surgery. Patients, who stop smoking benefit from long-term improvements to general health, decrease the risks associated with anaesthetic and have a better outcome from surgery. If you are interested in stopping smoking, please speak to your pre assessment nurse or GP for advice and services available.
Cancellation
If you are unable to attend your appointment, please contact us immediately so that we can offer your appointment to another patient.
Recovery after surgery
What may I experience after my operation?
- It is normal to experience some unusual sensation after surgery such as burning or tingling in your fingers and hand. Check your fingertips regularly during first 24 hours for normal pink colour, warmth and sensation.
- You may experience swelling in your fingers and hand after surgery this is normal. It is important to elevate the hand for the first 48 hours so that it is higher than the elbow. Avoid leaving it hanging down by your side for long periods.
- Should you have any bleeding, apply moderate pressure and raise your hand.
- It is expected you will have pain after the operation once the anaesthetic has worn off. You can take simple analgesia to help manage this.
- Pins and needles tend to resolve quickly but persistent numbness before surgery may never completely resolve.
- It is expected that your hand may be weak for 6 weeks after surgery. The wasting of the thumb muscles may improve but this takes months to years.
- Nerve recovery may continue for up 1 year following surgery. Both the speed of your recovery and how much your symptoms will improve are difficult to predict, and in some cases, recovery may not be complete. Most patients will notice an improvement in their condition with time following surgery.
Wound management
You will be advised when you can remove the wool and crepe bandage, this is usually after 48-72 hours. It is important to keep the wound and dressings dry until your wound check at your GP practice. This is usually 10-14 days after your operation. You will be informed if you have absorbable stitches or stitches that need to be removed. If you are unable to get an appointment at your GP surgery, please get in touch on the numbers provided at the end of this leaflet.
Contact your GP or get in touch on the numbers below if:
- You experience increasing pain, numbness or a change in colour of your hands
- Swelling or pins and needles in your hand that is not relieved by raising it, exercises or loosening the bandage
- You have pain that does not go away after pain relief or exercises
- Suspected wound infection – the wound becomes hot, red or produces a discharge
When can I resume normal activities?
You can use your hand straight away but you need to keep it clean and dry until the wound has fully healed. It will be at least 2 weeks before you can use your hand properly. Within the first 2 weeks, use your hand for light activities within the limits of your pain and swelling. Your hand will feel weak and uncomfortable initially. Avoid heavy gripping, lifting or repetitive use in the early stages of healing.
Work
You will usually need 1-4 weeks off work for light activities and office based work. Manual workers will be unable to return to work for a period of 6-8 weeks following the operation; this includes using vibration tools, heavy lifting or repeated loading of the hand and wrist. Heavy manual work may be longer. Discuss any concerns with the consultant or a member of the team.
Driving
Generally, you are safe to drive when your wound is healed and you are free of dressings, providing you can move your fingers, make a fist and your hand is not too painful or tender. You will need to assess you have full control of the vehicle. It is advised that you contact your insurance company.
Exercises
It is important that you exercise your hand as soon as possible after surgery. You can move the fingers within the constraints of the dressing. Ensure you are moving your elbow and shoulder to prevent stiffness.
Tendon Gliding
Perform the exercises below in sequence, 5 times each, every 2 hours until you can do them easily, are able to make a tight fist and can fully straighten all your fingers.

Touch the thumb to each fingertip, 5 x each

Place your elbow on a table, bend, and straighten your wrist, repeat x 5

Turn your palm towards the ceiling and then towards the floor, repeat x 5

Scar
Once the stitches have been removed and your scar has healed you can start massaging the area to reduce any tightness and thickening. It is important to care for your scar in the early stages after healing. Use an un-perfumed cream and rub in a circular motion over the scar. It is the massage of the underlying scar tissue which reduces the scaring not the cream itself.
The scar massage will help to speed up the flattening of the scar. If the scar is tender or sensitive to touch, it is important that you touch it lightly and gradually build up the pressure with the scar massage as it becomes more comfortable. It is normal for the scar to be very sensitive in the first 2-4 weeks after surgery and it will improve with massage. You can massage the scar for 2-3 minutes, twice per day for up to 3 months following the operation.