Welcome to the Colposcopy Clinic at the Queen Elizabeth Hospital in Gateshead. We look forward to welcoming you for your review. Please see the below information we have given you to assist or help with any concerns or question you may have throughout your care with us.
If you have any further questions – Please do not hesitate to contact the Colposcopy Team.
On this page
- Why have I been referred to the Colposcopy Clinic?
- What does an abnormal cell mean?
- What is a Colposcopy?
- What if I am currently pregnant?
- What can I do to prepare for my appointment?
- What happens before the examination?
- What happens during examination?
- What will my biopsy result show?
- What if I need treatment after a cervical biopsy?
- Pregnancy and LLETZ Treatment
- Test of cure (TOC) cervical screening
- How will I find out the result of my Biopsy?
- Where can I find out more information?
- Friends & Family Feedback
Why have I been referred to the Colposcopy Clinic?
You may be referred to the Colposcopy Clinic for one of the following reasons:
- Your cervical screening test has shown abnormal cells or the HPV virus,
- Your GP or Nurse is concerned about the appearance of your cervix,
- Your GP or Nurse has difficulty obtaining a cervical screening sample,
- You have irregular bleeding and/or bleeding after sexual intercourse,
What does an abnormal cell mean?
Cervical screening is not a test for cancer; it is a test to check the health of the cells of the cervix. Most test results show that everything is normal, but for around 1 in 20 of those with a cervix the test shows some abnormal changes in the cells of the cervix.
The reason most are referred to the Colposcopy Clinic is because a cervical sample result has shown abnormal cells, this is known as dyskaryosis. This could mean that there are pre-cancerous changes in the cells of your cervix (the neck of your womb). This is called Cervical Intra-epithelial Neoplasia (CIN).
These act as an early warning sign that cancer may develop in the future. They are usually caused by HPV (Human Papilloma Virus). Most of these changes won’t lead to cervical cancer and the cells may go back to normal on their own. But in some cases, the abnormal cells need to be removed so they can’t become cancerous.
Pre-cancerous cell changes or abnormalities:
- Low Grade Dyskaryosis High risk HPV+ve
Most cases of CIN 1 improve without the need for treatment, therefore monitoring is recommended unless persistent.
Sometimes, the cervical sample is reported as borderline changes. Borderline is between normal and mild, so it means almost normal but not quite. Low grade smears (mild and borderline) will very often revert back to normal without any treatment.
- High Grade Dyskaryosis High risk HPV+ve)
These changes have a higher tendency to develop into cancer, and may require a minor treatment. In some high grade (CIN2) cases monitoring of this change can also be an option.
- Endocervical or Glandular Intraepithelial neoplasia
These changes occur higher up in the inner cells of the cervix. CGIN is not cancer but these changes have a higher tendency to develop into cancer, therefore treatment is recommended.
It is important for you to attend your appointment so we can have a closer look at your cervix (the neck of the womb).
What is a Colposcopy?

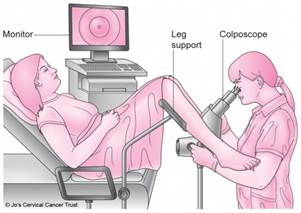
Colposcopy is an examination of the cervix, vulva or vagina using a colposcope (a colposcope is a type of microscope, It looks like a pair of binoculars on a stand – see these pictures above).
It helps identify any area on your cervix which may be abnormal. The colposcope does not touch you or go inside of you but allows the colposcopist to look at your cervix closely under magnification.
At the Northern Gynaecological Oncology Centre we have two ways of performing Colposcopy. The second type of Colposcopy is called DySIS (the picture on the right).
DySIS uses different colour filters and magnification options to create a digital image of your cervix and identifies changes on your cervix by showing a coloured map on a digital screen.
What if I am currently pregnant?

Please still attend your appointment – It is safe to do a colposcopy examination during pregnancy; however no biopsies or treatments would be routinely completed whilst you are pregnant.
Instead you will be monitored usually around early pregnancy and then at the end of your second trimester. A further review will be organised for any biopsies or treatments twelve weeks after your baby has been delivered as required. Please bring any maternity notes where possible so we can document your review in these too.
What can I do to prepare for my appointment?

You are more than welcome to bring a friend or relative with you to the Colposcopy clinic and they can also stay with you during your examination if you wish.
You can eat and drink as normal prior to your appointment. Please try to ensure you have had something light to eat and drink where possible prior to your review.
You may wish to wear comfortable clothing – to avoid removing all of your lower clothing during examination you may wish to wear a long loose skirt.
You may have a slight discharge after your appointment so you may wish to bring a sanitary towel – please note we also provide these in clinic for your comfort.
If you take medication to thin your blood (anticoagulants) such as Warfarin and Clopidogrel or Apixaban – please contact the Colposcopy Clinic or alternatively contact your GP Practice for advice prior to your appointment.

You may find taking simple over the counter painkillers such as Ibuprofen and/or Paracetamol tablets approximately one hour before your appointment may help. If you suffer with severe anxiety and feeling especially worried about your review, please speak to your GP prior to your appointment as they may be able to prescribe medication to aid with this. We do offer Entonox (this is an inhaled analgesic given in clinic) in clinic also for our patients to aid with making the examination comfortable.
Please bring simple OTC (over the counter) analgesics to your appointment should you feel you may need this after your review. You should always follow the instructions provided in the leaflet supplied with your medication.
What happens before the examination?

Before you are examined – the colposcopist will explain what your Cytology sample (cervical screening test) result means and what will happen during your examination.
The colposcopist will also wish to ask you some questions about your periods, what type of contraception you use as well as questions about your general medical, surgical and familial history. If you have any hip problems or recent hip surgeries please inform the doctor or nurse at your appointment – this is so we can ensure you are comfortable during examination.
Once this is complete and any of your questions you have are answered – You will be guided to a screened area in which you will be asked to undress form the waist downwards (a long loose skirt can stay on and be lifted up instead if preferred). You will have a sheet covering you whilst being examined.
What happens during examination?
The nurse assisting the colposcopist will help you to position yourself on a special type of couch. The couch has padded supports or foot rests on which you can rest your legs on. The nurse will stay with your during the examination to ensure you are comfortable and provide support.
When you are comfortable and ready to be examined – The Colposcopist will then gently insert a speculum into your vagina – just like when you had your cervical screening test. They will then look at your cervix using the conventional colposcope or the DySIS colposcope.
There will be a screen where you can watch the examination and procedure if you wish. In some occasions the colposcopist may want to ask your permission to take some pictures for medical records and teaching purposes. This is only a request and you can decline this.
The colposcopist will then apply one or two liquids onto your cervix which help to identify any areas of abnormal cells. Any abnormal areas will appear white. If any abnormal areas are identified the colposcopist may recommend a small sample of tissue – a punch biopsy – from this area. We also review the vagina with these liquids and sometimes we may see changes like above to this area.
The punch biopsy is very small – around the size of a nib of a pen or a small freckle. You will be asked to give a cough when the colposcopist is taking a sample. You may feel a slight stinging or ‘cramping’ sensation or discomfort but it should not be painful. Once the punch biopsy has been taken the colposcopist will stop any bleeding from that area by applying a small crayon with a chemical on the end which helps to stop the bleeding (silver nitrate) or by applying pressure with a piece of gauze.
Sometimes we place a small gauze like dressing over the area to help with the bleeding which will remain in place. If this is used you will be given advice on this at the end of your appointment.
If you have a small biopsy of the vagina – we will give a small amount of local anaesthetic to ensure this is more comfortable for you.
You will not need a local anaesthetic for this minor small biopsy procedure to the cervix, however if you require a LLETZ or Loop biopsy (a treatment) – local anaesthetic will be given.
A LLETZ/Loop biopsy (treatment) will be completed if required if the colposcopist identifies an area requiring this or if you have had a cervical biopsy showing pre-cancerous changes recommending this.
- In 1 in 100 to 14 in 100 women, infection of the cervix may cause heavy bleeding, an offensive discharge or pain and may require treatment with antibiotics
- Mild to moderate period like bleeding or a clear discharge may persist for four weeks after the procedure in 85 in 100 of women
- Heavy bleeding requiring further treatment such as vaginal packing or blood transfusion is rare but may be more common if you take blood thinning medication or if an infection develops following the procedure
- Removing these pre-cancerous changes will not necessarily remove the HPV virus and you will still be required to undergo your further screening as recommended which may involve further review back in Colposcopy if abnormal
It is also best to avoid heavy exercise, swimming and not to have sexual intercourse and using sanitary towels instead of tampons for the next four weeks following the procedure.
These measures allow the cervix to heal as quickly as possible and reduce the likelihood of infection.
You will be told what is normal during the healing process following a treatment and what may indicate you have an infection or heavy discharge.
You will be given an aftercare leaflet also with information as well as contact numbers in case you have any concerns when you are at home.
We are a training trust and we may occasionally have trainee medical and or nursing staff in the clinic. You will be informed if this is case to ensure you would be happy with this prior to you going into the consult room.

Occasionally you may wish to let someone else drive you home as the local anaesthetic can make you feel a little shaky initially as this contains adrenaline. Alternatively you can stay in clinic until you feel safe to drive.
If you had a punch biopsy then blood stained discharge should be very slight and will last for around two to five days. You will need to use towels rather than tampons during this time and refrain from intercourse to allow the biopsy site to heal. You should feel well enough after your examination to continue with your usual routine.
You will be told what is normal during the healing process following a biopsy and what may indicate you have an infection or heavy discharge. You will be given an aftercare leaflet also with information as well as contact numbers in case you have any concerns when you are at home.
What will my biopsy result show?

Your biopsy result (the sample of tissue) will show how abnormal the area is and will indicate if treatment is needed.
Normal or HPV
A normal test result or those showing high risk HPV (Human Papilloma Virus) means no abnormal cell changes have been found. No action is needed and you don’t need another cervical screening test until it is routinely due.
HPV is a transient common virus which affects around 80% of males and females. There is no treatment and most will clear this virus with the help of the immune system. HPV (human papillomavirus) is transmitted by sexual skin-to-skin contact which means that penetration is not required to contract the virus.
The type of HPV which is associated with the development of abnormalities (pre-cancerous changes) on the cervix has no symptoms so women (and men) are unaware of the presence of the virus and most women may have had the virus for many years before it was detected. Due to most men and women being exposed to HPV – you don’t need to confront or blame your current or previous sexual partner. We would however recommend smokers to stop – as smoking can weaken the immune system meaning some will hold onto the virus for longer.
Inadequate
Sometimes you may be told you need to have a repeat colposcopy and/or biopsy because the first biopsy could not be interpreted properly.
This may be because:
- not enough cells were collected from the two cell types on the cervix
- the cells couldn’t be seen clearly enough
- an infection was present
You’ll be asked to come back so another sample of cells can be taken – This may not be straight away. This is to allow the cervix to heal adequately and for cells to regenerate prior to a further biopsy.
CIN or CGIN
If you have pre-cancerous cell changes your follow up will be as below;
- CIN1 means that only a third of the cells in the abnormal area are affected. These may be left to return to normal and if the colposcopist feels your cervix shows this abnormality when examined they may take a small punch biopsy.
- CIN2 means that up to a third of the cells in the abnormal area are affected. The colposcopist will offer a treatment or in some cases discuss conservative management/surveillance of these changes as these can sometimes improve without treatment.
- CIN3 means that all the cells in the abnormal area are affected and treatment will be usually be advised if these cell changes are seen.
- CGIN means that the cell changes are present higher up in the inner cells in the cervix and treatment of this is also advised.
Only very rarely will a biopsy show cell changes that have already developed into a cancer. Very early stage cervical cancer can be treat with a LLETZ/loop excision.
What if I need treatment after a cervical biopsy?
If your biopsy has shown CIN 2 or 3 we will contact you by telephone or invite you back to clinic via letter to discuss the results and the treatment going ahead.
If you have CIN3 or CGIN we usually treat this area by a loop or LLETZ treatment. This allows us to remove the cells affected whilst causing minimal disruption to the surrounding normal tissue.
If you have CIN2 – there are two possible options of managing or treating this.
Conservative management
Local audit from 2023 shows 82% of those with a cervix with CIN2 improve these changes without the need for a LLETZ/loop treatment. If you have CIN2 and the clinician feels this may be a suitable management option.
You will be discussed at our colposcopy MDT meeting – this is attended by a team of experts to review your cervical screening and or biopsy result and collectively we decide on reviewing your results if this is a suitable management for you and discuss this decision with you.
If this is a suitable option for you – you will then be seen for a minimum of two years every six months for repeat cervical screening and a colposcopy review with cervical biopsies. If the changes are improving then this is positive and you may be suitable for discharge after two years. Sometimes we may decide to continue to monitor you further if felt required. We discuss all ladies at the end of their two year follow up back at our Colposcopy MDT (Multi-disciplinary team meeting).
If the changes are shown to not be not improving or perhaps worsening – or if there were any concerning clinical symptoms, then we would undertake a loop or LLETZ/loop treatment.
LLETZ/Loop treatment
This is the recommended management for High Grade CIN or CGIN via our NHSCSP guidelines. A LLETZ or loop treatment is completed in clinic under local anaesthetic. Occasionally, this may be required to be completed under a general anaesthetic.
This treatment involves removing a small amount of tissue from the surface of the cervix under local anaesthetic. The procedure once we have examined you takes only a few minutes within your clinic appointment.
- In 2 in 100 to 14 in 100 patients undergoing LLETZ, cervical stenosis (scarring) or narrowing of the opening of the cervix can occur. This can rarely cause pain during periods, difficulty getting pregnant or
- problems with future screening tests as it can be more difficult to access and review the canal (the inside cells) of the cervix
- In 1 in 100 to 14 in 100 women, infection of the cervix may cause heavy bleeding, an offensive discharge or pain and may require treatment with antibiotics
- Mild to moderate period like bleeding or a clear discharge may persist for four weeks after the procedure in 85 in 100 of patients
- Heavy bleeding requiring further treatment such as vaginal packing or blood transfusion is rare but may be more common if you take blood thinning medication or if an infection develops following the procedure
Pregnancy and LLETZ Treatment
In 2 in 100 to 14 in 100 patients undergoing LLETZ, cervical stenosis or narrowing of the opening of the cervix can occur. This can rarely cause pain during periods, difficulty getting pregnant or problems with future screening tests.
Around 2 in 100 people who become pregnant after LLETZ will give birth before 37 weeks (prematurely) because of the treatment. This is more likely if you have had LLETZ more than once or had more than 10mm of your cervix removed. Most LLETZ treatments remove less than 10mm of your cervix.
We recommend if you become pregnant following a LLETZ to advise your midwife of your previous treatment(s). Rarely will a cervical suture during pregnancy be required after a single LLETZ treatment. (This can be used to help support the cervix).
Test of cure (TOC) cervical screening
All women who have been treated for CIN or CGIN will have a cervical screening test performed six months following their treatment – this is usually completed with your Practice Nurse/GP in the community.
If high risk HPV is not detected (Negative) patients are discharged back to ‘normal’ recall (three or five years).
If HPV is detected patients are referred directly back to colposcopy – Please remember approximately 80% of patients will pass TOC cervical screening (this means it is negative) and therefore will not be referred back to colposcopy.
Your date for this will be included in your results letter and you will receive a reminder from the national cervical screening service.
How will I find out the result of my Biopsy?

We will write to you with the result of your biopsy usually within four-six weeks. We will also explain if we need to see you again or if we can discharge you so you can have any future cervical screening samples at your GP practice with your GP or Practice Nurse.
Your sample(s) or tissue may be stored to allow us to check your test results again, if needed, at a later date. Sometimes samples taken may be used for teaching, research or public health monitoring in the future interests of all NHS patients. Samples kept for this purpose will not identify you. You have the right to refuse consent for samples of your tissue to be used for teaching or research purposes. If you refuse consent; this will not affect your treatment in any way.
Where can I find out more information?

If you would like any further information before you come to Colposcopy your Practice Nurse will be happy to discuss your abnormal cervical sample result. You can also contact the Nursing team in Colposcopy who will be happy to discuss any concerns or answer questions you may have – Please contact 0191 445 6178 or our secretary on 0191 445 6270
Further information can be found on the following website: www.joscervicaltrust.org
Friends & Family Feedback
We value your feedback and wish to make your visit to our service as positive as possible for you.
Please complete one of our Friends and Family postcards or alternatively respond to the trust text message after your visit in clinic and direct them to the post box provided at the entrance/exit to our clinic.