Subacromial decompression Surgery
This leaflet aims to help you understand and gain the maximum benefit from your operation. It is intended for patients who are either thinking about or have decided to have surgery after discussing this with their consultant or surgical team. Each person’s operation is individual and you may be given specific instructions that are not contained in this leaflet.
The shoulder
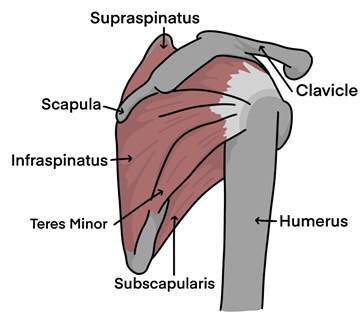
The shoulder is a ball and socket joint, it is the most mobile joint in the body. It depends on strong muscles and ligaments to move and stabilise it. The most important muscles for this are the rotator cuff, this is a group of muscles that work together to move the shoulder. They originate from the shoulder blade, their tendons form a hood covering the humeral head (ball) of the shoulder joint. The tendons pass under a bony arch called the acromion and are protected by a small cushion called a bursa.
The four rotator cuff muscles are individually called; subscapularis, supraspinatus, infraspinatus and teres minor.
What is subacromial pain?
This generic term describes any of the structures that sit within the shoulder and can cause pain. It can also be known as rotator cuff tendinopathy or rotator cuff related pain. It is a common shoulder problem that can develop gradually or quite quickly if the arm has been used for an over demanding activity or if there is weakness in the rotator cuff muscles.
It usually responds well to conservative management like exercise and physiotherapy, which can help to address the motor control around the shoulder. Symptoms normally improve within 6 to 12 weeks by doing simple exercises, although in some instances, it may take many months of rehabilitation for pain to settle. Physiotherapy can also help you manage your pain and advice on how to improve your overall general health and well-being.
What are the symptoms?
- Pain – is around the shoulder and in the upper arm. It can spread further down the arm and up towards the neck and shoulder blade. It is often worse on movement particularly moving the arm away from the body, reaching up, lifting activities or placing the hand behind the back. It can also be painful when in bed whilst sleeping on the affected side.
- Stiffness – can occur over time if movement is avoided due to pain levels.
- Loss of movement and function
What are the treatment options?
The treatment options for managing a painful shoulder are:
- Pain killers are commonly advised, your pharmacist or GP can discuss this with you.
- Leaving it alone – there is the option of not having surgery. We are unable to predict if your pain will get better or worse, but modifying your painful activity may help, especially in the early stages.
- Physiotherapy can be excellent at helping you to improve your movement and build muscle strength, which aids recovery and function. This may take time but gradually your symptoms may improve to a comfortable level.
- Steroid Injections – are offered to patients when significant pain is the main symptom, physiotherapy is not helping or if patients are not suitable for surgery. Pain relief following injections is usually temporary and this does differ patient to patient.
- Surgery – maybe recommended when the above measures have failed and patients have undergone an appropriate course of physiotherapy, which is ineffective in helping the shoulder symptoms. The decision to proceed with surgery is an individual choice made between you and your consultant or part of the team. Not everyone with shoulder pain requires surgery.
Surgical procedure
The purpose of the operation is to increase the subacromial space in which the rotator cuff tendons move. A surgical drill may shave away part of the ligament and some of the bone underneath the acromion. The inflamed bursa may also be removed. This increased space will allow the tendons to move more freely, thereby aiming to reduce the mechanical and painful irritation of the structures in the shoulder.
During your operation, other common additional surgical procedures will likely take place depending upon the findings;
- Debridement (clean up) of tendons or tendon repair. If a tendon repair, this would mean longer in a sling and more post-operative precautions/restrictions.
- Tendon release being a biceps tenotomy. This is cutting off the long head of biceps tendon which is a common procedure. This will change the appearance of your upper arm muscle in that the biceps will sit lower called a ‘popeye’ sign.
- Capsular release – this can help to improve the underlying stiffness and movement of the shoulder.
Surgery is usually performed as a keyhole procedure (arthroscopic), this type of surgery has quicker recovery times. This surgery will require 2-3 small incisions, which will leave small scars. The surgeon can use these incisions to place a small camera inside the shoulder as well as the instruments to perform the surgery.
Are there any complications with this operation?
The intended benefits of the operation are to improve pain and function, although all surgical procedures are associated with a degree of risk. The main complications are:
- Pain is common after this operation and vary for each individual depending upon pain thresholds, the nature of the problem and various other factors. It can be common to have significant pain for the first 6 weeks following surgery and through the night. There is also the risk that you may not get full pain relief following your operation or your pain may worsen.
- Stiffness – In most cases, post-surgical shoulder stiffness improves, although in some cases you may need additional intervention.
- Infection of the wound is uncommon (<1%). You should contact the surgeon if you get a temperature, notice discharge from your wound, feel unwell, or if your wound becomes red, sore or painful.
- Bleeding (<1%)during or after surgery.
- Neuro vascular nerve injury is uncommon (< 1%). Numbness and pins and needles are the usual symptoms. Most nerve injuries usually resolve in time, however permanent nerve damage may occur.
- Unsightly scarring – most surgical scars look a bit red following surgery but usually they have disappeared to a thin pale line by 1 year.
- Failure to fully resolve symptoms
- May need further surgery
- Deep Vein Thrombosis (DVT) or Pulmonary Embolism (PE). A DVT is a blood clot in the leg and the clot can spread to the lungs (PE) and make you unwell. These are uncommon.
- Anaesthetic complications – the anaesthetist will discuss this with you.
What happens before the operation?
Pre-admission assessment
This is an assessment of your health to make sure you are prepared, for your admission, treatment and discharge. Please bring a list of all your current medication including a list of allergies and the type of reactions. Before the date of your admission, read very closely, the instructions given to you by the pre-admission assessment and your appointment confirmation letter.
Planning ahead
Once you have your date for surgery, you can do several things to aid preparation for your operation and to improve your recovery.
It is important to plan and arrange for how you will manage when home. Stocking up your freezer with easy cook items is advised (particularly if you live alone), as you may find daily tasks such as cooking more difficult initially after your operation. If you have family or friends, who can stay with you or visit regularly, this may make your recovery easier both for helping with household tasks and moral support.
Smoking
Smoking has been shown to delay wound healing and increase complications after surgery. Patients, who stop smoking benefit from long-term improvements to general health, decrease the risks associated with anaesthetic and may have a better outcome from the operation. If you are interested in stopping smoking, please speak to your pre assessment nurse or GP for advice and services available.
Weight
Even though you may feel fit and healthy at your current weight, patients with a higher body mass index are most likely to experience potential serious complications both during and after surgery. If you are keen to lose weight, please speak to your GP or pre assessment nurse for services available.
Cancellation
If you are unable to attend your appointment, please contact us immediately so that we can offer your appointment to another patient.
Your surgery
Anaesthetic
Subacromial decompression surgery is usually performed under a regional anaesthetic (nerve block) with or without a general anaesthetic (which puts you to sleep). A regional anaesthetic will numb the affected arm and will assist with pain control after the operation. It can take up to 24 hours before this completely wears off, during this time, you will not be able to move your arm and you may have some altered sensation of the arm or hand that persists for some weeks. During this time, you will need to wear the sling until the block has worn off. The anaesthetist will see you before your operation and discuss your anaesthetic with you.
Day of surgery
You will be given specific instructions about when to stop eating and drinking, please follow these carefully, otherwise this may pose an anaesthetic risk and we may have to cancel your surgery. You should have a bath or shower before coming in to hospital. The anaesthetist, surgeon or a member of the team will visit you prior to the operation, and can answer any questions. You will be asked to sign a consent form.
Prior to and during the operation, a blood pressure cuff is placed on your arm, some leads placed on your chest and a clip attached to your finger. This will allow the anaesthetist to check your heart rate, blood pressure and oxygen levels during the operation. You might just receive an injection into the side of your neck (nerve block) to numb your shoulder; you will remain awake during the procedure. If you have a general anaesthetic, a needle will be put into the back of your hand to administer the drugs to send you to sleep.
Hospital stay
Subacromial decompression is a day case surgical procedure, however depending on your recovery after the operation and your home situation; you may be required to stay overnight.
Recovery after surgery
After surgery, you will have sutures to close the wound and a dressing in place. Your arm will be in a shoulder sling.
You will see a physiotherapist in the recovery room. They will give you advice regarding your surgery and provide you with a post-surgical exercise leaflet. It is important you do these exercises regularly to prevent your shoulder from becoming stiff.
When do the sutures come out?
The sutures are removed at your GP surgery, usually 10-14 days after your operation. Keep the wound dry until it has fully healed.
Pain
Significant pain and discomfort is common after surgery, especially the first 6 weeks. You will be given appropriate painkillers on discharge from hospital. If you feel you are unable to manage your pain, please discuss this with your GP, surgeon or physiotherapist.
Wearing a sling
On return from theatre, your shoulder will be in a sling to give your arm support and help with pain. The sling is usually worn for comfort until the nerve block resolves. You can take it on and off as you wish once the nerve block wears off, aiming to discard it within a few days. It may be more comfortable to wear this on a night for a little longer if the shoulder is uncomfortable. If you have any additional procedures like a rotator cuff repair, then the sling will need to be worn for longer, and you will be advised of this.
If you are unsure, please contact your consultant’s secretary or the physiotherapy team before discarding the sling.
Sleeping
We would recommend that you lie on your back or on the opposite side. You should not lie on your operated shoulder as this may increase your pain. If you are lying on your back to sleep, placing a pillow under your upper arm/elbow can make it more comfortable. When lying on your non-operated side, you can fold or hug a pillow in front of you to support the arm. You can also tuck a pillow along your back to help prevent rolling onto the operated shoulder.
Washing and dressing
When washing and dressing sitting down is usually best as you can support your arm on a pillow. You may find it easier wearing loose clothing with front fastenings. When getting dressed, dress your operated arm first and when undressing this arm comes out last.
Physiotherapy
You will be referred to out-patient physiotherapy and an appointment will be sent out in the post. The physiotherapist will progress your exercises and assist in your recovery. Continuing the exercises at home will enable you to gain maximum benefit from your operation. This may continue for many months until both you and the physiotherapist are happy with your progress.
If you have not received a physiotherapy appointment within 2 weeks of your operation, please contact the physiotherapy team on the number(s) below.
Physiotherapy locations
Please note, depending on the location of your GP, the physiotherapy provider may be different:
- If you have a Gateshead / Newcastle GP, your physiotherapy provider will be Tyneside Integrated Musculoskeletal Service (TIMS). If you have a query about your first appointment with TIMS, please contact the booking team on 0191 445 2643
- If you have a Durham GP, your physiotherapy care will come under Durham. Please contact the Queen Elizabeth hospital, physiotherapy department should you not receive your first appointment on 0191 445 2320
- If you have a GP that is outside of the Gateshead / Newcastle or Durham area and you have had elective surgery, your physiotherapy will be at the Queen Elizabeth hospital. If your surgery is due to trauma, your physiotherapy provider will be with the hospital affiliated to your GP practice. Should you not receive your first appointment, please contact physiotherapy reception on 0191 445 2320
Driving
We advise that you do not drive for at least 2 – 4 weeks after your operation. You must be out of your sling, feel comfortable, and be in complete control of the vehicle. It is wise to discuss this with your insurance company before you return to driving.
Flying
Discuss with your consultant and with the airline’s medical department if you wish to fly within 6 weeks of your operation due to the risk of clot formation.
Your recovery
The recovery time after a subacromial decompression is variable for each individual. It is expected that you will make a full recovery within 6 to 9 months following the operation, with most of the improvement being achieved in the first 3 months.
Functional activities (these are minimum times and could be longer)
| Return to work | Office work | as tolerated, 2 – 4 weeks |
| Manual Job | 3 months, you may need to modify activities or repetitive overhead activity | |
| Swimming | Breaststroke | as able |
| Freestyle | 12 weeks | |
| Golf | 6 weeks | |
| Lifting | as able, guided by pain | |
| Specific sport | be guided by physiotherapy / surgeon |
Telephone numbers
| During the hours of 8am – 8pm contact the Day Surgery Unit, Peter Smith Surgery Centre, Queen Elizabeth Hospital | 0191 445 3009 |
| During the hours of 8pm – 8am contact Level 3, Peter Smith Surgery Centre, Queen Elizabeth Hospital | 0191 445 2028 |
| During the hours of 08:00 – 16:30 contact the Physiotherapy Department | 0191 445 2320 |
| During the hours of 8am – 8pm. If you have a Gateshead or Newcastle GP, TIMS will be your physiotherapy provider. If you have a query about your first appointment with TIMS please contact our booking team on 0191 445 2643 If you are a current TIMS patient and have a query about your follow-up appointment please contact our local admin team on 0191 213 8800 | Booking Team: 0191 445 2643 Local Admin Team: 0191 213 8800 https://www.tims.nhs.uk/ |
| Main Switchboard | 0191 482 0000 |