What is the Critical Care Department?
Critical care provides closer monitoring and treatment that is more intensive to patients who require it. This can be after an operation or serious illness. Patients are categorised as level 2 or level 3 depending on their needs. Level 2 patients (high dependency) have one nurse caring for two patients and level 3 patients (intensive care) have one nurse caring for one patient.
Staff in Critical Care
Doctors working in critical care are usually anaesthetists; however, other professionals from a wide variety of disciplines will visit the department. These include physiotherapists, dieticians, pharmacists, speech and language therapists and other specialist nurses. They all work closely to plan, implement specialised treatment, and care for our patients.
All staff can be identified by their name badges and uniforms
Some of the Critical Care team

Our philosophy
We believe that the patients in our care are treated and respected as unique individuals.
Throughout this period of their illness, it is our intention to provide a high standard of care appropriate to the patients’ needs, to encourage and support family involvement and to accommodate their mutual support.
We seek to provide clear information, respecting the individual’s right to confidentiality when communicating with the multidisciplinary team, the patient and their family.
Whilst we strive to achieve our patients full recovery and return to their best level of health, we also realise this is not always possible. In this event, it is our aim to ensure a peaceful and dignified death in keeping with the patients’ cultural and spiritual background.
What happens when a patient arrives on the department?
Many admissions are of an urgent nature and the doctors and nurses will be very busy treating the patient. You will be able to see the patient at the earliest opportunity but your patience is appreciated.
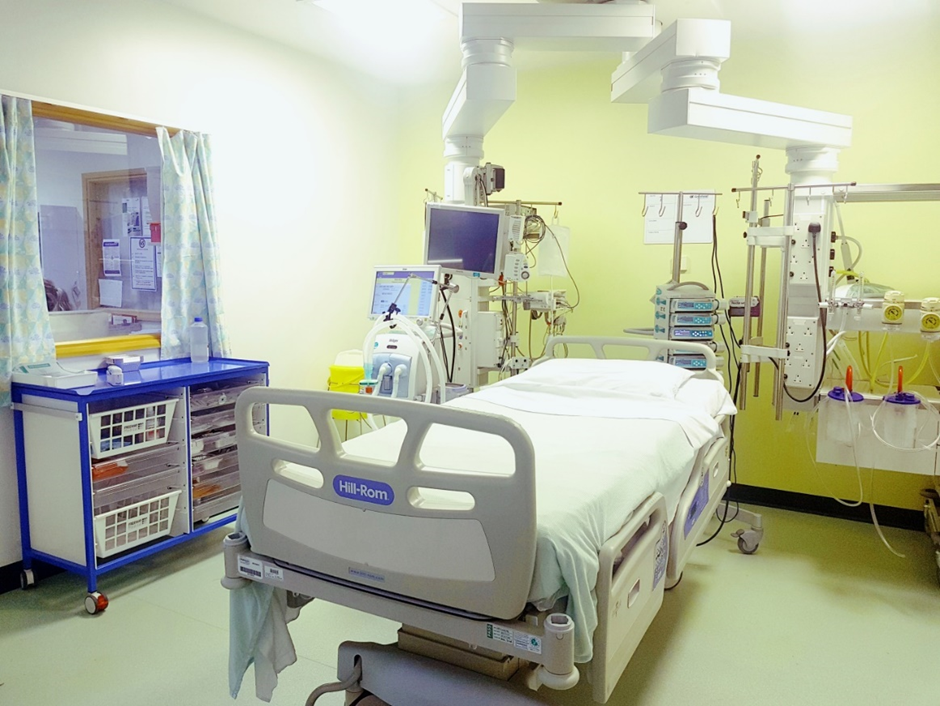
Critical care can be a daunting place. There is a lot of equipment around the bed space and many unfamiliar sounds. Your relative may look very different to how they normally look. They may be connected to one or more types of monitor to allow staff to observe and measure a variety of functions such as heart rate, blood pressure and oxygen. A number of infusion pumps are usually in use and are to administer specific amounts of fluids and drugs through small tubes into veins.
An Intensive care patient may be having support from a breathing machine (ventilator). To do this the patient will have a tube in their mouth going down their windpipe (trachea) and to ensure they are not distressed, they will be given sedation. During this time, they may not be able to respond to you and will not be able to talk, however they may be able to hear you.
How you can help
- Talking to them as normally as possible
- Bring in their favourite music to be played quietly
- Ask if you can be involved in some basic nursing care if that’s what the patient wouldn’t normally mind
- Hold their hand. If you are unsure about touching the patient, ask the nurse for advice.
If your relative is on a ventilator for three days or more, we will start a photo diary. This is to help the patient make sense of what has happened to them. The staff looking after your relative will write in the diary and you are invited to write in it as well if you wish. Photographs will be taken at particularly important points in their stay and stored safely for the patient.
Later, if the patient wants to, the rehabilitation team can go through the diary and answer any questions they may have. We just keep one hard copy of the photos and it is up to the patient if they want to see them or not, if they do not give consent to see the photos the photos are kept for one year and then destroyed along with the diary.
It is the job of the nurses and staff to explain what is happening and to reassure you. Please feel free to ask questions at any time. If the patient’s admission to critical care is planned, we recommend that you ring the department on the day before making your journey. We will then be able to advise you as to the best time to visit.
What will the patient need?
Your relative may stay on critical care for as little as one day to as long as several weeks, depending on their illness and response to treatment. During this time, we will ask you to provide the patient with:
- Deodorant, shaving foam, and hair comb. We provide special antiseptic wash, which will reduce bacteria on the skin and reduce infection.
- One set of comfortable day clothes and a couple of nighties or pyjamas. (We initially use gowns as they help when there are a lot of tubes attached to the patient)
- Dressing gown and well fitted slippers
- Glasses, dentures and hearing aids if worn normally (really important when the patient is waking/ awake)
- Newspaper/book/tablet computer
- Small amount of food i.e. sweets/ drinks etc.
It is advisable to keep the patients property to a minimum due to limited space.
The hospital cannot accept responsibility for items left in the department unless handed to the nursing staff for safekeeping.
Where are we?
The critical care department is situated in the ‘Red’ zone, level 3 of the Surgical Block. It is well signposted.
Visiting
We operate an open visiting policy and you are welcome to visit your relative throughout their stay. Patients are encouraged to rest to aid their recovery. Please respect the need for rest for both your relative and other patients during your visit.
Restrictions to visiting will be effected in the event of Covid. Please ask the Nurse in charge for up-dates regarding this.
If you have a visitor’s passport, you may be entitled to additional benefits and facilities. A visitor’s passport is an agreement with staff, to make your loved ones time in hospital more comfortable, for example, you may get help with meals, parking and access to the ward. Please ask the nurse in charge for details.
We allow two visitors at the bedside at one time. Please do not bring hot drinks and food into the department unless prior arrangement has been made with the nurse in charge. This is to avoid accidents and reduce infection risks.
The use of mobile phones is not permitted for relatives. This is to ensure patient confidentiality and reduce the risk of interference with some electrical equipment. Please read the notices on the entrance.
An intercom system is used to access to the department. Use the relevant button for access to your relative i.e. Level 3 or Level 2. A member of staff will check if it is appropriate to allow entry and let you in. Outside coats need to be removed and can be stored in lockers provided in the waiting area (£1 refundable deposit) Please wash your hands when entering and leaving the department and comply with any extra precautions as applicable.
Children Visiting
Children are welcome to visit the critical care department; however, please give this some thought, as it can be a stressful environment.
They should only visit immediate family members and staff should know in advance so waiting time can be kept to a minimum.
Visits by children should be kept to five to ten minutes at a time. Additional information and resources are available to help children when visiting critical care. Please ask the nurse in charge.
If you are feeling unwell, please avoid visiting. Critical care patients are especially vulnerable making them more prone to infection. If you need advice, please ring before visiting. Again, Covid restrictions may apply.
Waiting
If you are asked to wait, there is a waiting area outside of the department.
It is not unusual to have to wait for long periods of time, as most patients require help with almost all aspects of living/care. With this in mind, here is an outline of the department’s usual activity:
These times are approximate and may vary. It does not mean you cannot visit but please be aware that you may be asked to wait.
- 07:30-08:00 Nursing and medical staff handover
- 09:00- mid-morning: Doctors review each patient and ward round
- 09:00-late morning: personal care/ washing patients
- 09:30-11:00: Physiotherapy
- 12:00-13:00: patient lunchtime
- 13:00-15:30: Physiotherapy
- 18:00-18:30: patient dinnertime
- 19:30-20:00: Doctors handover
- 20:00-20:30: Nurses handover
- 20:00-22:00: Doctors evening ward round
Planning for discharge
The decision to discharge your relative to the ward will be made when their condition stabilises and improves. Our acute response team will continue to support their care on the destination ward. The rehabilitation team will assess and provide the appropriate level of care to the patient and will also contribute to the continuation of care in order to achieve the patients’ optimal level of independence.
It may take up to 18 months to fully recover and people may experience physical and psychological problems. Some patients will be invited to a follow up outpatient’s clinic with the critical care rehabilitation nurse and physiotherapist two to three months after they have returned home. If your relative has not been invited but you or your relative have questions or concerns related to recovery or their time in critical care, please contact the critical care rehabilitation nurse on 0191 4453210.
Hospital facilities
Quiet rooms are available for private discussion with the doctor.
Toilets are outside of the department, just before the visiting room.
Public telephones are at the main hospital entrance.
Shops: Amigos, Subway and Costa coffee shop.
ATM is situated in Amigos.
Other catering facilities
The Hub near the Windy Nook entrance for a full range of homemade hot and cold items open Monday to Friday 8.30am – 4pm.
Peter Smith Surgery Centre cafe opens 8.30am – 4.30pm Monday to Friday for hot and cold drinks, sandwiches, scones and jacket potatoes with an area to sit outside.
Outpatients shop and café.
Parking
The Trust now operates a parking eye, and you will need to pay for your stay when you leave. Machines are located near the main entrance at A+E and in the car parks. If you have a relative in critical care for a long time, you may be able to get a parking permit. Please ask the nurse in charge.
Public transport
Travel information can be found on the Nexus website www.nexus.org.uk or by telephoning 08706082608.
Taxi
Direct line telephones are located at the main entrance to the hospital.
The Trust operates a No Smoking policy throughout its buildings and grounds. We thank you for your co-operation.
Chaplaincy
Visitors are welcome to the hospital chapel. It is located next to Quenellies and accessible at any time. If your relative would like to be visited by a hospital chaplain or have other cultural or religious needs, please talk to a member of the nursing staff.
Research and Audit
To improve patient care, evaluate our service and plan for future development, the department plays an active role in audit and research. You may be approached to consider being part of a research trial but this is voluntary. For further information, please ask for an explanatory leaflet.
Translators
Please ask the nurse taking care of your relative if you wish to access this service.
Fire procedure
Fire alarms are tested regularly. In the event of a fire/ emergency, please follow instructions from staff.
The Patient Advice and Liaison Service (PALS)
PALS can:
- Advise and support patients, their families and carers
- Provide information on NHS services to help you make choices
- Listen to your questions, suggestions, concerns and compliments
- Help sort out problems quickly on your behalf
- Guide you through the different services available through the NHS
Tel: 0191 445 6129 or email: [email protected]
Suggestions and Comments
Whilst we endeavour to ensure the highest possible standard of care and service, we would appreciate any suggestions or constructive criticisms you may have regarding the facilities available or the care we provide. Most issues can be resolved through discussion with the Nurse in charge however if you feel this is not possible then please use the PALS.
Contact Details
Direct line contact to:
- Intensive Care: 0191 4452007
- High Dependency: 0191 4452008
Enquiry calls may be made to the department at any time, however, please note that any information given over the phone can only be very general. Any changes in condition and treatment will be explained more fully when you visit. Due to the confidential nature of medical records, detailed information is usually only given to the patients’ next of kin or nominee.
Please remember that every phone enquiry takes staff away from the bedside. If the patient has a large family and / or many friends who might telephone, we recommend that one or two people are nominated to ring and pass on the information to others.